Thyroid Cancer Overview
Incidence in Australia
According to the most recent data available from the Australian Institute of Health and Welfare, thyroid cancer is the 9th most common cancer. It accounted for 2% of all new cancer cases diagnosed in Australia in 2013, but accounted for 3.8% of new cancers in women. This equates to one woman in 75 being diagnosed with thyroid cancer before the age of 75 years, and 1 in 65 women before the age of 85 years.
The incidence of thyroid cancer in Australia is also increasing significantly, increasing from 2.7 to 12.3 cases per 100,000 population from 1982 to 2017 (Fig. 1). This represents a 351% increase in incidence over this time. The increase in thyroid cancer may be due to an increase in medical surveillance and the introduction of new diagnostic techniques, such as neck ultrasonography (Vaccarella et al. 2016).
This is especially so in women, where in the the last 5 years thyroid cancer has moved from 10th most common to 7th on the list of top ten cancers in all age groups. In men, it is the 18th most common cancer.
In addition, analysis of the age groups affected show that thyroid cancer in 2016 was estimated to be the third most commonly diagnosed cancer in women aged between 15 and 24 years, and the fourth most common in the 25-59 year age group.
 Fig. 1: Estimated percentage change in age-standardised incidence rates, Australia, 1982 to 2017 (Source: AIHW Australian Cancer Database 2013)
Fig. 1: Estimated percentage change in age-standardised incidence rates, Australia, 1982 to 2017 (Source: AIHW Australian Cancer Database 2013)
There were 3154 new cases of thyroid cancer diagnosed in Australia in 2017, but only 361 new cases in 1982, nearly an 8-fold increase of thyroid cancer cases in 35 years. The number of new cases of thyroid cancer in women was nearly three times that for men, with 879 in men (6.9 per 100,000) and 2275 new cases in women (17.5 per 100,000).
Overall, the age-standardised incidence rate for thyroid cancer for all persons has increased from 2.7 to 12.3 cases per 100,000 in that time, and the number of new thyroid cancer cases is increasing at about 5% per year.
The incidence is shown on the AIHW graphs below (Fig. 2), which confirm the rising incidence of thyroid cancer, but also illustrate the very low overall mortality rates in thyroid cancer in Australia. The second graph on the right shows the variable rates of thyroid cancer incidence in different age groups in the latest years of data available.
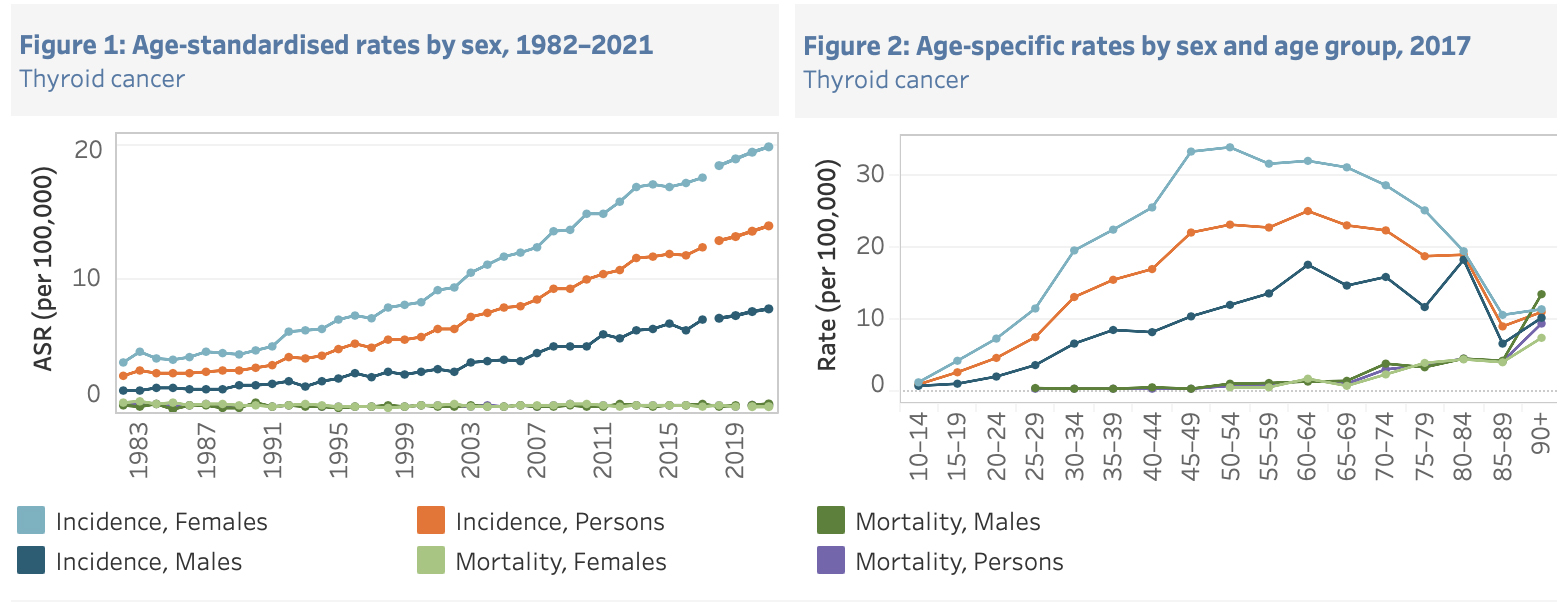 Fig. 2: Thyroid cancer incidence and mortality rates, 1982-2017, with projections to 2021 (left) and Thyroid cancer incidence (2017) and mortality rates by age group (Source: AIHW Australian Cancer Database 2017, AIHW National Mortality Database)
Fig. 2: Thyroid cancer incidence and mortality rates, 1982-2017, with projections to 2021 (left) and Thyroid cancer incidence (2017) and mortality rates by age group (Source: AIHW Australian Cancer Database 2017, AIHW National Mortality Database)
Incidence in Victoria
The age-standardised incidence rate of thyroid cancer in Victoria in 2019 was 11.4 new cases per 100,000 for females, and 5.4 for males, for a total of 739 cases. There were more than double the number of cases in women (501) than in men (238) (Fig. 3).
By 2030-2034 however, the number of thyroid cancer cases in Victoria is projected to rise to 1362, with a continuing increase in the incidence rate in both sexes. The projected incidence is expected to rise to 20.6 cases per 100,000 women and 9.4 per 100,000 men, which is just over 2:1.
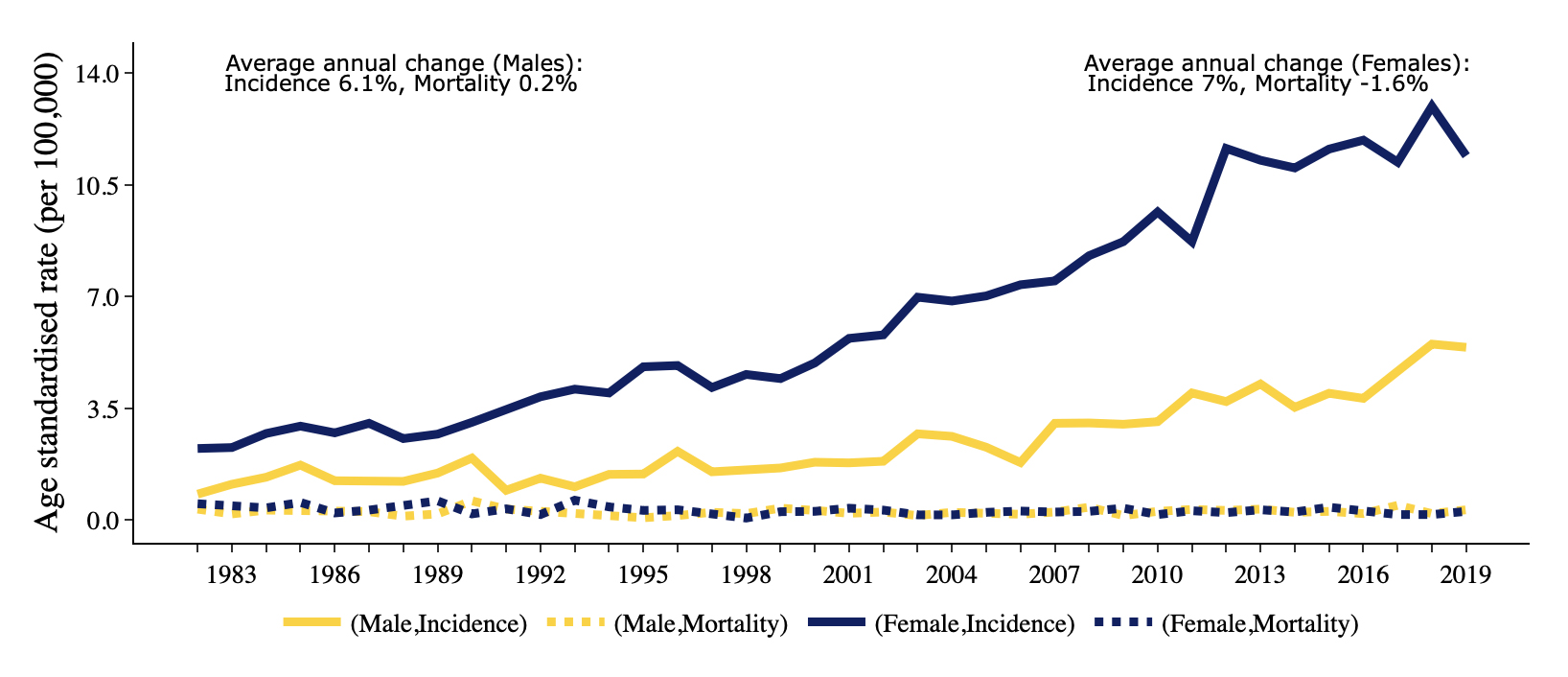 Fig. 3: Thyroid cancer in Victoria, Australia 1982-2019 (Source: Victoria Cancer Registry 2019)
Fig. 3: Thyroid cancer in Victoria, Australia 1982-2019 (Source: Victoria Cancer Registry 2019)
Although thyroid cancer can occur in all age groups, it tends to favour younger age groups than other cancers, like colon or breast cancer (Fig. 4). In fact, in 2019 it was the second most common cancer in women aged 15-24, and the 4th most common in women aged 25-59 years.
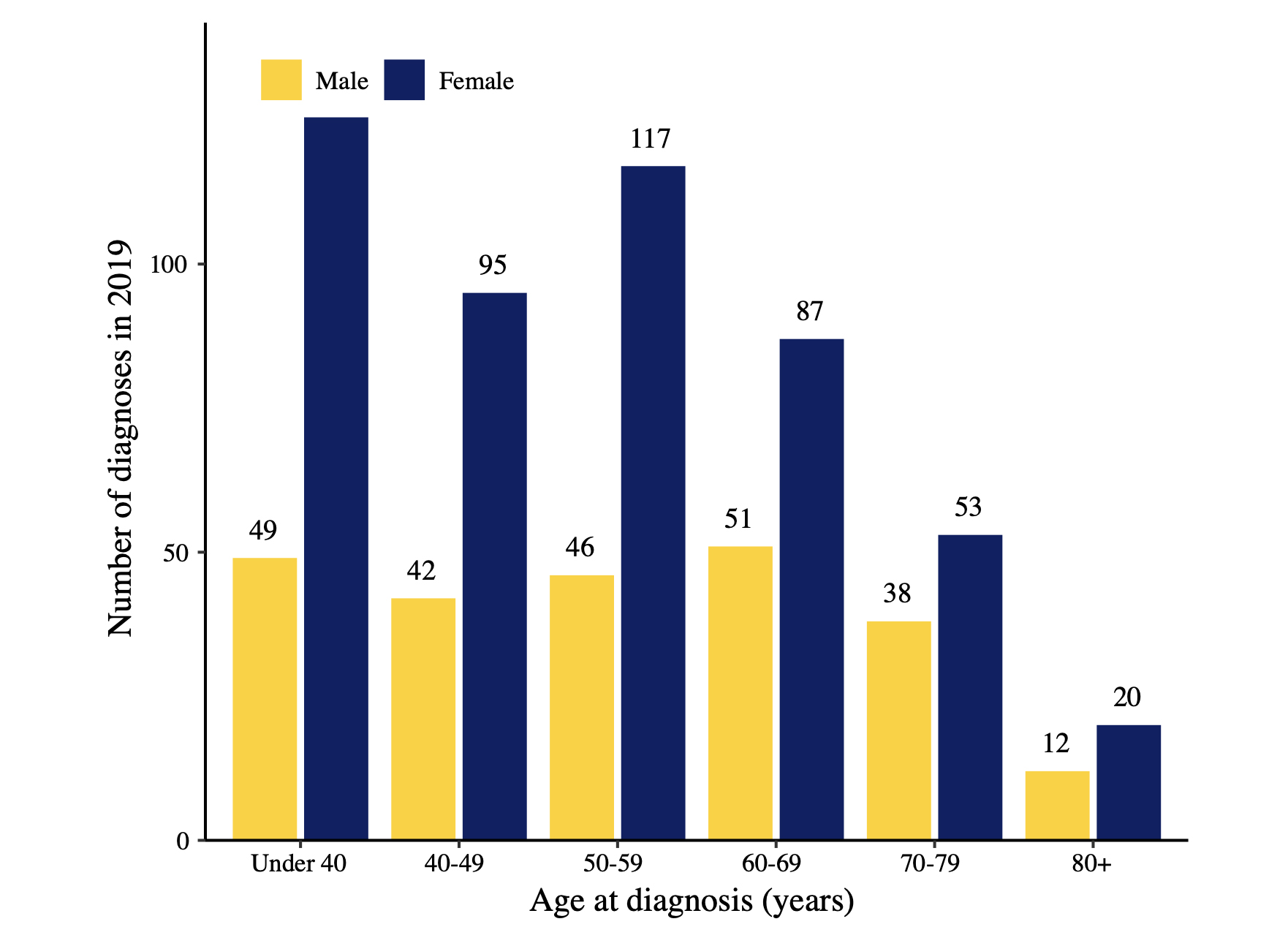 Fig. 4: Age-specific thyroid cancer cases in Victoria 2019 (Source: Victorian Cancer Registry)
Fig. 4: Age-specific thyroid cancer cases in Victoria 2019 (Source: Victorian Cancer Registry)
Deaths from thyroid cancer remain very low however, with an incidence of only 0.3 per 100,000 in males and 0.3 per 100,000 in females.
The increasing incidence of thyroid cancer was thought to be due to better detection with high resolution ultrasound and image-guided FNA cytology, implying that smaller tumours should be found more often. This is not the whole answer however, as a study in the USA of the incidence of thyroid cancer from 1988 to 2005 showed that the incidence rates of differentiated thyroid cancers of all sizes increased during that time in both men and women.
The increased incidence across all tumour sizes suggested that increased diagnostic scrutiny is not the sole explanation, but that other explanations, including diet, environmental influences like radiation exposure, and molecular pathways, should be investigated.
Types of Thyroid Cancer
There are five main types of thyroid cancer:
- Papillary (>80%)
- Follicular (10%)
- Medullary (7%)
- Anaplastic (2%)
- Lymphoma (<1%)
Papillary and follicular thyroid cancers arise from follicular cells, as do anaplastic thyroid cancers. Medullary thyroid cancers arise from the parafollicular cells and lymphomas arise from the stroma.
Squamous cell carcinoma (SCC) of the thyroid is extremely rare (less than 1% of thyroid cancers). The tumours often tend to be advanced at presentation, and have been reported to resemble the clinical behaviour of anaplastic carcinoma. The tumour seems to have a poor response to radiotherapy, but long-term survival is possible if the disease is diagnosed early and is completely resected.
In addition, the thyroid can be the site of metastases (secondary spread of cancer) from other tumours elsewhere in the body, such as renal cell cancer (kidney), breast, lung and colon cancer. Metastases to the thyroid are rare, and are usually associated with other metastases elsewhere in the body. They may appear many years after treatment of the primary cancer, and are usually easily diagnosed by FNA cytology (needle biopsy).
Clinical features
Typical presentations are listed below, but there are a lot of conditions that can also have these symptoms besides thyroid cancer:
- lump or swelling in the neck
- difficulty breathing or shortness of breath
- difficulty swallowing (dysphagia)
- a change in the voice
- a cough that will not go away
- enlarged lymph nodes in the neck, usually on one side only
Thyroid cancer usually presents with a nodule or lump in the thyroid (Fig. 5). This may be either as a single nodule in an otherwise normal gland, or when one nodule in a goitre grows bigger and becomes more obvious (dominant). It is also possible for thyroid cancer to present with symptoms related to secondary spread of cancer, such as bone pain or a spontaneous fracture.
 Fig. 5: Thyroid nodule left side of neck
Fig. 5: Thyroid nodule left side of neck
The clinical features vary depending on the time of presentation. An early presentation may be with just a neck lump and no symptoms. A later presentation may have additional features of hoarseness (due to pressure on the recurrent laryngeal nerve) or difficulty in swallowing and eating.
It is important to realise that thyroid nodules are common, and it has been estimated that about 10% of the population will have them, but less than 3% of all thyroid nodules are malignant.
Management of thyroid cancer
The management of all forms of thyroid cancer follows certain principles and has the following aims:
- remove all of the tumour
- minimise morbidity (complications)
- stage the disease
- facilitate postoperative therapies e.g: radioactive iodine, thyroxine suppression
- permit long-term surveillance
- minimise the risk of recurrence or the development of metastases
Prognosis of thyroid cancer
The overall prognosis of thyroid cancer is the best of all the other cancers, and Australians have a better survival than most on an international comparison. In 2016, there were 140 deaths from thyroid cancer (66 men and 74 women, accounting for only 0.5% of all cancer deaths in Australia. Relative survival rates have also markedly improved: in 1982-1987 5-year survival was 83.5% but in the period from 2011-2015 had increased to 96.6%. In women this figure is even higher at 97.8%. Thyroid cancer is not in the top 20 causes of death in either males or females in Australia.
Thyroid cancer survival sits at or near the top of the 'league table' of survival for all cancers in Victoria (Figs. 6 & 7). In 2016 there were only 32 deaths from thyroid cancer across Victoria, and the death rate has been decreasing steadily for some time.
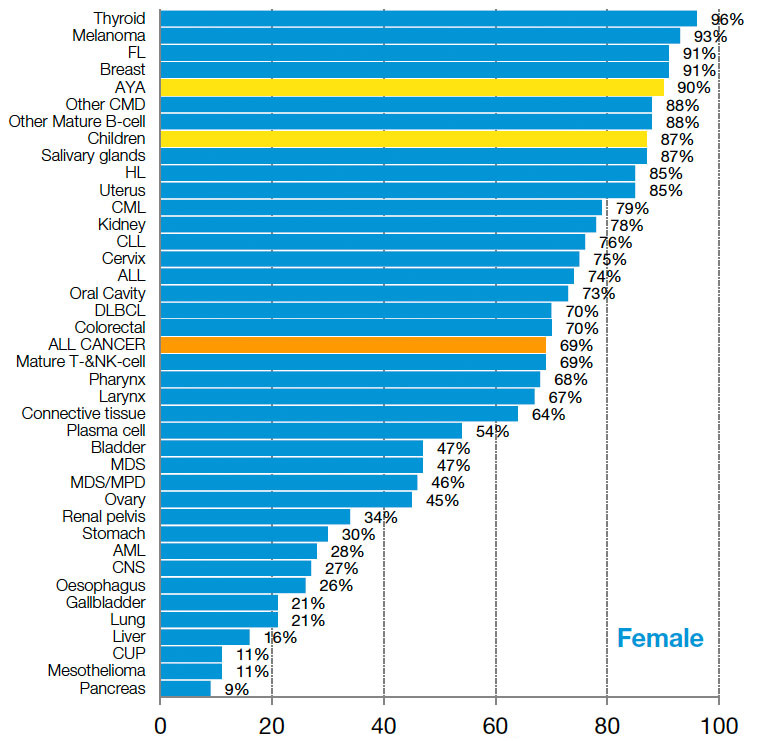 Fig. 6: 5-Year-Survival by cancer type for Victorian women with cancer 2011-2015. (Source: Canstat Victorian Cancer Registry 2017)
Fig. 6: 5-Year-Survival by cancer type for Victorian women with cancer 2011-2015. (Source: Canstat Victorian Cancer Registry 2017)
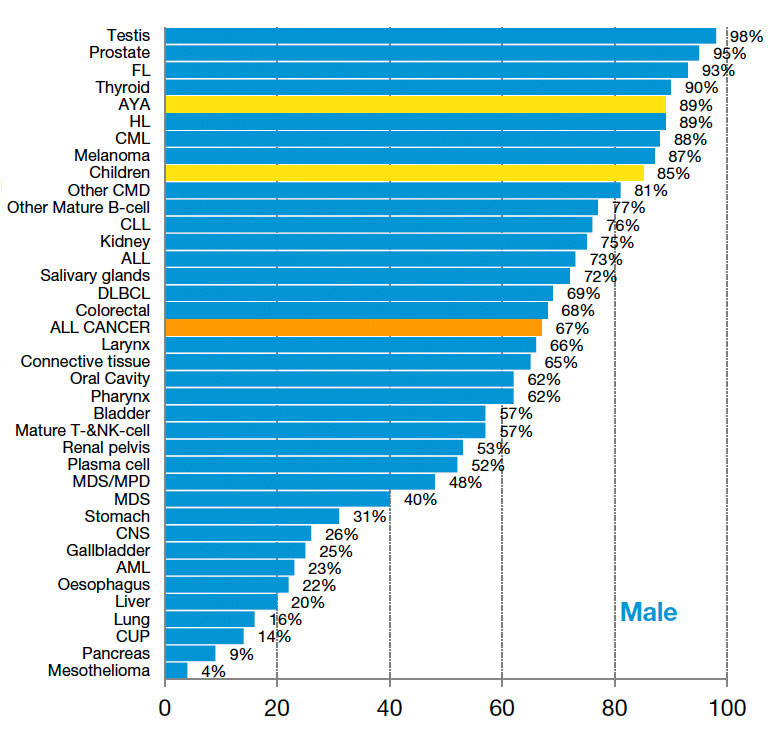 Fig. 6: 5-Year-Survival by cancer type for Victorian men with cancer 2011-2015. (Source: Canstat Victorian Cancer Registry 2017)
Fig. 6: 5-Year-Survival by cancer type for Victorian men with cancer 2011-2015. (Source: Canstat Victorian Cancer Registry 2017)
Overall 5-year survival rate for thyroid cancer in Victoria is about 96%, having improved from only 84% in 1990 (that is that 96% of all patients with thyroid cancer will still be alive after 5 years). Survival in 2014 was 93% for males, and 97% for females, the best for any cancer. This compares very favourably with England and Europe, which have much lower survival rates, and with the USA where survival is only slightly better.
In addition, the younger the patient presents with thyroid cancer, the better the survival, with rates over 98% in Australian patients under the age of 40 years.
The survival rates for thyroid cancer also depend on the type of tumour. The most common types of thyroid cancer (Papillary and Follicular) have the best prognosis, with cure rates in the younger age group as high as 99%, and for the older patients still 96%.
Medullary cancer has a slightly worse prognosis, but there is still a 90% 5-year survival in Victoria. It is more aggressive and tends to spread to lymph nodes at an early stage. Anaplastic thyroid cancer has the worst prognosis of all the thyroid cancers as it often presents after it has spread widely in the neck and elsewhere in the body, and it grows rapidly. An operation is rarely able to remove the entire tumour, or even possible.
The prognosis for any given thyroid cancer patient depends mostly on what type of cancer it is, where it is located and if it has spread outside the thyroid, the age of the patient at diagnosis and whether the patient is male or female.
However it is important to note that up to 30% of cancers can recur, often many years after treatment. For this reason, patients with thyroid cancer need life-long follow up checks to make sure that the cancer does not come back or spread elsewhere.
I have created a booklet, outlining the steps in diagnosis and treatment of thyroid cancer, which can be found on the webpage Guide to Surgery.