Fig.1: Left hemithyroidectomy specimen containing a minimally invasive FTC presenting as a lump on the left edge of the thyroidFollicular Thyroid Cancer (FTC)
Fig.1: Left hemithyroidectomy specimen containing a minimally invasive FTC presenting as a lump on the left edge of the thyroidFollicular Thyroid Cancer (FTC)
Follicular cancer of the thyroid is much less common than papillary cancer (10%), and has a higher incidence in areas of iodine deficiency (25-40%). The peak incidence is in an older age group (mean age 50 years) but like PTC it affects women three times more commonly than men.
FTC is a well-differentiated tumour, encapsulated, solitary, exhibiting capsular and vascular invasion, and it spreads via the blood stream. It rarely spreads to the lymph nodes of the neck, which tends to occur late in the disease.
Pathology
This is a malignant epithelial tumour with evidence of follicular cell differentiation without the features of papillary cancer. The lesion is usually solid, occurs predominantly in women, approximately 10 years later than papillary cancers. There are two types, based on the degree of invasiveness of the lesion.
Minimally invasive FTC (MIFTC)
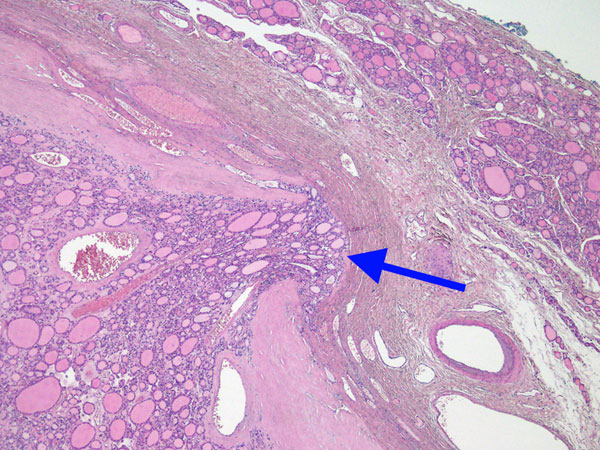 Fig.2: Minimally invasive FTC with a tongue of capsular invasion (arrowed). Photo Dr Chris DowThis is a solid, encapsulated, fleshy tumour that looks very much like a simple thyroid adenoma. The capsule tends to be extremely thick and irregular when compared with that of a simple adenoma.
Fig.2: Minimally invasive FTC with a tongue of capsular invasion (arrowed). Photo Dr Chris DowThis is a solid, encapsulated, fleshy tumour that looks very much like a simple thyroid adenoma. The capsule tends to be extremely thick and irregular when compared with that of a simple adenoma.
As the lesion increases in size, transgression of the capsule is more likely, so that the incidence of follicular cancer is around 30% in lesions greater than 3cm in diameter.
Diagnosis is made by observing capsular invasion, requiring the pathologist to carefully inspect the whole capsule (Fig. 2). For this reason diagnosis is usually made on paraffin section (formal pathology), as determining capsular invasion is very difficult at frozen section. There can also be difficulty following fine-needle aspiration to distinguish traumatic capsular rupture from true foci of capsular invasion.
This tumour has an excellent prognosis, and as a result it is possible to treat low risk MIFTC (small tumours in younger female patients) with limited surgery (lobectomy), as for small papillary cancers.
Widely invasive FTC
 Fig.3: Widely invasive FTC with vascular invasionThis shows widespread infiltration of blood vessels, the capsule and adjacent thyroid tissue. (Fig. 3) It can on occasions have no capsule whatsoever.
Fig.3: Widely invasive FTC with vascular invasionThis shows widespread infiltration of blood vessels, the capsule and adjacent thyroid tissue. (Fig. 3) It can on occasions have no capsule whatsoever.
The structural features are variable, but there is always a follicular element. There are no nuclear changes suggestive of papillary cancer, as if this was present it would suggest this to be a follicular variant of papillary thyroid cancer (FVPTC).
Follicular cancer does not invade lymphatics and spreads by the bloodstream to the lungs, bones and less frequently to the brain. Immunostaining for thyroglobulin is usually positive in this tumour.
This type of tumour is highly aggressive and needs to be treated with great care because there is a 50% mortality as compared with the minimally invasive tumour where there is only a 3% mortality. The separation of the two entities is crucial and emphasizes the need for a pathologist with a special interest in endocrine pathology.
Presentation
Follicular cancer of the thyroid presents in two ways:
1) As a single lump in the thyroid:
This is the usual mode of presentation, like its more common cousin, papillary cancer (Fig. 4). It will be felt as a lump in the neck, and may cause pressure symptoms, such as difficulty in swallowing or breathing. Often it is first noticed by a relative or friend, or the GP, rather than by the patient.
 Fig.4: Specimen of FTC in right lobe presenting as a lump in the neck; left thyroid is normal
Fig.4: Specimen of FTC in right lobe presenting as a lump in the neck; left thyroid is normal
2) As pain in a bone or a spontaneous fracture:
When follicular tumours spread by the bloodstream they may present with symptoms related to secondary deposits, which may occur in lungs, brain or in the bones. In the latter case the bone is softened by these deposits of tumour and may fracture, or lead to spinal cord compression and paralysis (Fig. 5).
 Fig.5: MRI scan of an FTC secondary deposit in the spine (left), wrapping around the spinal cord (right)
Fig.5: MRI scan of an FTC secondary deposit in the spine (left), wrapping around the spinal cord (right)
Diagnosis
Diagnosis is made in a similar way to PTC with a combination of clinical suspicion, FNA cytology and imaging (see PTC Diagnosis).
The major problem with follicular cancer is actually making the diagnosis before operation. Unless there is definite evidence of secondaries, it is virtually impossible to differentiate between a non-malignant and malignant follicular lesion on fine needle aspiration. This is because the diagnosis is made by seeing capsular and vascular invasion under the microscope, something which is not possible with FNA, which will only give cellular information. This means that at operation only 20% of follicular tumours will actually turn out to be cancer.
A number of attempts have been made to improve the accuracy of FNA in follicular tumours using molecular markers and different immunostains without much success.
Treatment
Like in papillary thyroid cancer, the management of FTC comprises a four-pronged attack:
- Thyroid surgery
- Radioactive iodine therapy (+/- external beam radiotherapy)
- Drug treatment - Thyroxine therapy
- Regular follow-up
The goals of therapy also remain the same: to eradicate the primary tumour, reduce the incidence of local and distant recurrence, minimise complications, facilitate treatment of metastases and arrange long term surveillance.
I have also created a booklet, outlining the steps in diagnosis and treatment of thyroid cancer, which can be found on webpage Guide to Surgery.
Thyroid surgery
The American Thyroid Association Guidelines released in 2015 recommended the following:
- FNA cytology showing a follicular lesion (Bethesda classification) usually mandates lobectomy as the least surgical procedure, although in some cases a different operation may be indicated
- Frozen section examination is unhelpful when the FNA diagnosis is that of a follicular lesion
- If definitive histology reveals a follicular adenoma or a hyperplastic nodule, no further treatment is required
- FTC under 1 cm in diameter with minimal capsular invasion should be treated by lobectomy alone
- Patients with FTC showing high risk features, such as size >4cm, vascular invasion, or metastases to nodes or elsewhere in the body, should be treated by total thyroidectomy, and most will also have radioiodine ablation
- Patients with FTC >1cm and <4cm without extrathyroidal extension, and no metastatic disease can be treated by lobectomy or total thyroidectomy; lobectomy in low-risk patients may be sufficient but this will depend on disease features and patient preferences - a slightly 'grey area'
- Palpable/suspicious cervical lymph nodes are dealt with in a similar manner to papillary carcinoma
The choice between total thyroidectomy and lobectomy for a follicular lesion (diagnosed on FNA) will depend on the discussions between the patient and surgeon. Performing total thyroidectomy has the advantage that no further surgery is required if the lump is cancer, but the disadvantage of this approach is that if the tumour is benign the patient will need to go on lifelong thyroxine, which may not have been necessary if limited surgery had been performed (lobectomy).
Partial thyroidectomy (lobectomy) has the advantage that in benign lumps no more needs to be done, but the disadvantage that in the case of cancer a second operation to remove all remaining thyroid tissue may be required (completion thyroidectomy). However this can be achieved with no greater morbidity than a total thyroidectomy performed as a single procedure.
Radioactive iodine
Treatment with radioactive iodine and external beam radiotherapy is as for papillary cancer.
Drug therapy
Treatment with thyroxine aims to achieve the same result as in papillary cancer.
Follow-up
While most patients are cured by their treatment, thyroid cancer can recur or spread to other parts of the body, even many years after surgery. That is why regular follow up checks are needed for life, especially in the first 5-10 years after surgery when the risk of the cancer returning is highest.
There are a number of tests that are used to monitor progress:
- Thyroglobulin blood test
- Thyroid function test (to monitor thyroxine replacement levels)
- Ultrasound
- occasionally, Whole body scan
Thyroglobulin blood test
A thyroglobulin (Tg) test measures the level of thyroglobulin in the blood. It is generally performed once or twice a year during follow up, unless it is abnormal, when more frequent estimation may be done.
Thyroglobulin is a protein in the blood that stores thyroid hormone. Because thyroid cells (and thyroid cancer cells) are the only cells in the body that make thyroglobulin it is a very accurate measure of whether thyroid cancer cells are present somewhere in the body. If the Tg is elevated, then investigation by ultrasound or whole body scan is used to check for the source of the excess thyroglobulin.
 Fig.6: US showing enlarged lymph nodes containing thyroid cancerTg is usually measured while the patient is still taking thyroid tablets (so that the TSH is still suppressed), but occasionally it can be necessary to perform a ‘stimulated Tg’ by doing the test while the TSH is elevated. This is achieved by either stopping the thyroid tablets for a few weeks, or by using recombinant human TSH (rhTSH) or ‘Thyrogen’.
Fig.6: US showing enlarged lymph nodes containing thyroid cancerTg is usually measured while the patient is still taking thyroid tablets (so that the TSH is still suppressed), but occasionally it can be necessary to perform a ‘stimulated Tg’ by doing the test while the TSH is elevated. This is achieved by either stopping the thyroid tablets for a few weeks, or by using recombinant human TSH (rhTSH) or ‘Thyrogen’.
Thyroid function tests are regularly performed to make sure that the amount of thyroxine tablets is sufficient to replace the function of the thyroid and to suppress the TSH below the normal range, to minimise the risk of recurrence of the cancer.
Ultrasound
An ultrasound of the neck is usually done once a year in the first few years as a routine, looking for recurrence of the cancer and enlargement of lymph nodes (Fig. 6), which might indicate spread of the cancer. It also allows for a FNA biopsy to be done of anything suspicious.
In low risk patients the combination of stimulated thyroglobulin measurement and high resolution neck ultrasound has a 97-98% sensitivity to detect disease and 95-96% negative predictive value. Those low risk patients with undetectable thyroglobulin and negative ultrasound do not require further routine whole body scanning during followup.
High or intermediate risk patients may derive some value from a further whole body diagnostic scan at 6-12 months after ablation.
Other Tests
Occasionally other tests besides the ultrasound will be required, especially if there is evidence of recurrence.
A whole body scan (WBS) requires the patient to swallow a pill or liquid that contains a small amount of radioactive iodine and then lie down under a large camera that takes a scan of the whole body. If any thyroid or thyroid cancer cells are present they will show up as ‘hot spots’ on the film.
PET scanning is another form of whole body scanning using sophisticated nuclear medicine techniques, which is very effective in locating thyroid cancer cells. It is usually only used when there is evidence of disease on other tests.