Cushing's Syndrome (Hypercortisolism)
 Fig.1: Harvey CushingThis is the most common of the functional tumours of the adrenal gland.
Fig.1: Harvey CushingThis is the most common of the functional tumours of the adrenal gland.
First described by Harvey Cushing in 1932 (Fig. 1), Cushing's Syndrome describes a characteristic set of clinical features and biochemical changes due to chronically raised levels of the glucocorticoid, cortisol.
Cushing's syndrome occurs in all races. It affects more women than men, in a ratio of 3 to 1. It mainly occurs in those between the ages of 20 and 60 years, and has an incidence of between 0.7 and 2.4 cases per million people each year, so is a rare disease.
It is important to draw attention to the distinction between Cushing's syndrome and Cushing's disease. Cushing's disease is one of the causes of Cushing's syndrome. It describes the excessive secretion of adrenocorticotrophic hormone (ACTH) by small benign tumours found in the anterior pituitary gland. The terms Cushing's disease and ACTH-dependent Cushing's syndrome are used synonymously.
Causes
1. Excessive glucocorticoid administration
High doses of steroids (e.g for rheumatoid arthritis) is by far the most common cause of Cushing's syndrome, and can be readily diagnosed from a careful medication history.
2. ACTH-dependent Cushing's syndrome (80-85% of endogenous cases)
Excess ACTH stimulates the adrenal gland to over-produce cortisol.
Cushing's disease: Accounts for approximately 70% of organic cases. The most common cause is an ACTH-secreting microadenoma in the anterior pituitary gland. Rarely, macroadenomas are seen.
Ectopic ACTH syndrome: Involves tumours occurring outside the pituitary secreting ACTH, such as small-cell bronchogenic carcinoma, bronchial carcinoid tumours, and other neuroendocrine tumours. They account for 10% of organic cases of Cushing's syndrome.
Ectopic CRH syndrome: This is very rare with tumours occurring outside the hypothalamus producing corticotrophin releasing hormone (CRH), which raises ACTH levels and therefore cortisol levels. They account for less than 1% of organic Cushing's syndrome.
3. ACTH-independent Cushing's syndrome (15-20% of endogenous cases)
The adrenal gland autonomously produces excess cortisol as a result of a tumour or hyperplasia.
Adrenal adenoma: These are benign tumours of the adrenal gland secreting cortisol. They are generally larger than 2cm, unilateral, and are the most common cause of ACTH-independent Cushing's syndrome, accounting for 10% of organic causes of Cushing's.
Adrenal carcinoma: These are malignant tumours of the adrenal cortex producing, amongst other hormones, cortisol. Often androgens may be produced as well resulting in hirsutism and virilisation of women. Normally they are large tumours, > 6cm in diameter. They are very rare in adults, accounting for 8% of organic causes of Cushing's, but occur more commonly in children.
Macronodular adrenal hyperplasia (AIMAH): This is non-tumorous excessive growth of the adrenal gland, where the resulting nodules secrete cortisol. The aetiology of this is still to be determined. It accounts for <2% of organic causes of Cushing's.
Pseudo-Cushing's syndromes
This is Cushing's syndrome associated with alcoholism and/or depression in patients. It accounts for 2% of the causes of Cushing's syndrome. Blood and urinary cortisol levels may be raised and a disturbed circadian rhythm is often seen. Stopping alcohol consumption or treatment of the depressive disorder will result in cortisol levels returning to normal.
Symptoms of Cushing's syndrome
Most patients do not present to the doctor with the classical features of Cushing's syndrome (detailed below) but the majority in fact present with the more subtle features of subclinical Cushing's syndrome. Patients with subclinical disease have at least two biochemical abnormalities in their pathway of cortisol metabolism, but lack the overt clinical symptoms and signs of hypercortisolism. These patients are being picked up earlier because of the precision of laboratory and imaging studies now available.
Patients with subclinical disease will often present with features of the 'metabolic syndrome', a group of conditions exascerbated by the excess cortisol. The syndrome includes hypertension, poor glucose tolerance or diabetes Type II, poor bone density and increased fracture risk, abnormal serum lipids and obesity. Up to 20% of patients with an adrenal incidentaloma (incidentally found adrenal mass) will have subclinical Cushing's syndrome.
If obese patients with poorly controlled type II diabetes and hypertension are screened for Cushing's syndrome, the prevalence ranges from 2-5%.
Cushing's syndrome is associated with significant long-term morbidity and mortality, with a recent study showing that patients with incompletely controlled Cushing's syndrome had an 11-fold increase in mortality.
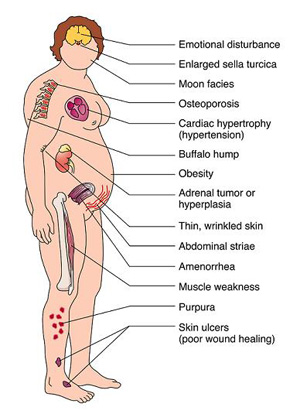 Fig.2: Main clinical features of Cushing's syndrome (from Nursingcrib.com)The classical symptoms and signs of Cushing's syndrome affect all parts of the body, giving patients with longstanding disease a characteristic appearance. Nevertheless, diagnosis depends on a high index of suspicion as changes may be subtle and slow. The main clinical features (Fig. 2) and their frequency are:
Fig.2: Main clinical features of Cushing's syndrome (from Nursingcrib.com)The classical symptoms and signs of Cushing's syndrome affect all parts of the body, giving patients with longstanding disease a characteristic appearance. Nevertheless, diagnosis depends on a high index of suspicion as changes may be subtle and slow. The main clinical features (Fig. 2) and their frequency are:
- 95% weight gain around the central regions (centripetal obesity)
- 90% facial plethora (red face)
- 90% change of appearance / moon face / ‘buffalo hump’
- 90% poor libido
- 85% thin skin
- 70-80% growth arrest in children
- 80% menstrual irregularities
- 75% hypertension
- 75% hirsutism (excessive hair growth) / acne
- 70% psychiatric problems: anxiety / depression / psychosis
- 65% easy bruising
- 60% glucose intolerance / diabetes
- 60% muscular weakness
- 50% back pain/ fracture
- 50% nephrolithiasis (kidney stones)
Next page: Cushing's syndrome diagnosis